Jon Anderson was a former track and field state champion and Footlocker Cross-Country Finalist. I had the opportunity to sit down and chat with him about his struggles, surgery, and rehabilitation process with Haglunds Deformity.
Interview with Jon Anderson (CLICK ME)

I would like to share some key things that I thought were especially important from this interview.
Diagnose the cause not the symptoms
Take the time to listen to the history of the injury. How and when did it happen? By taking this valuable time, you will give the patient a better opportunity to heal and restore functionality. I know from personal experience with my athletes, treating the symptoms typically will only make them feel good temporarily.
Listen to your patient
Jon like many other people who visit healthcare professionals felt as though he was not being listened to. John said, “it was frustrating getting misdiagnosed so many times. I would tell the PT I have been doing glute activation drills for a year or more and it wasn’t working, and they would just accuse me of not putting the time or work into my recover”
Don’t push through the pain
Maybe Jon’s surgery could have been prevented if he didn’t continually run through this pain. In the track world this is all too common; runners feeling something and ignoring initial symptoms. Most athletes HATE the idea of taking time off, however if you were to ask Jon what he would do differently, I’m sure he would say longer periods of rest. Check out my post on resting.
Anyone with a high arch is a candidate for Haglunds Deformity?
Not necessarily, however according to Lakeview Health, “high arches can contribute to Haglund’s deformity. The Achilles tendon attaches to the back of the heel bone, and in a person with high arches, the heel bone is tilted backward into the Achilles tendon. This causes the uppermost portion of the back of the heel bone to rub against the tendon. Eventually, due to this constant irritation, a bony protrusion develops and the bursa becomes inflamed. It is the inflamed bursa that produces the redness and swelling associated with Haglund’s deformity”(https://www.lakeviewhealth.org/upload/docs/HaglundsDeformity.pdf)
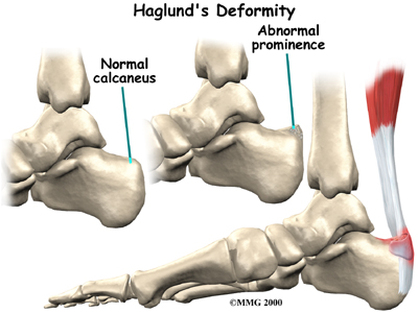
Haglunds Deformity: It will present on an x-ray as a hook-like structure. Can be incredibly painful if not diagnosed early enough.

Post Surgery
Just because you have had a recent surgery (and this does not only pertain to Haglunds) ask your doctor or physical therapist for ways to mobilize the surrounding connective tissue (muscles, joints, tendons, ligaments, cartilage etc). In Jon’s case, toe curls and light mobilization exercises helped speed his recovery (see video’s below). Post surgery is often a time for a person to become immobile.
Video’s of Jon’s Rehabilitation
https://www.youtube.com/watch?v=zShF9nuwbbs – Increasing circulation (Exercises that Jon did while in a cast) that helped speed up the recovery process.
https://www.youtube.com/watch?v=vx7U-J09kTU – Low-intensity occlusion training. Occlusion training means the act of causing a blockage of blood to the muscle groups being exercised with the use of cuffs, bands, or wraps. The term “occlusion” has a literal definition of “a closure or blockage.”
Check out Jon Anderson’s Blog and Website!

Hi David. Sorry to say I didn’t listen to the whole interview, but I know Jon’s brother so it was pretty funny to see him on a blog I read. Just wanted to point out your link to his blog has a typo. It should be redlegrunners (not reglegrunners). I’m also someone who has experienced physical therapy at the hands of someone who didn’t listen to me and actually made me worse. Then again I’ve had 3 other therapists who were excellent. I’m working with one right now who sees me 1-on-1 for a full hour which is amazing.
I spent a year in PT school, so I know how intense it is. Good luck to you!
LikeLike
David, thank you for your interview with Jon! It’s encouraging to see good information on the web that may positively influence another athlete’s choices.
LikeLike